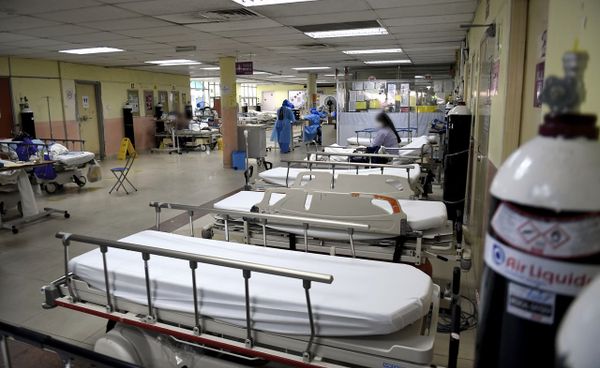
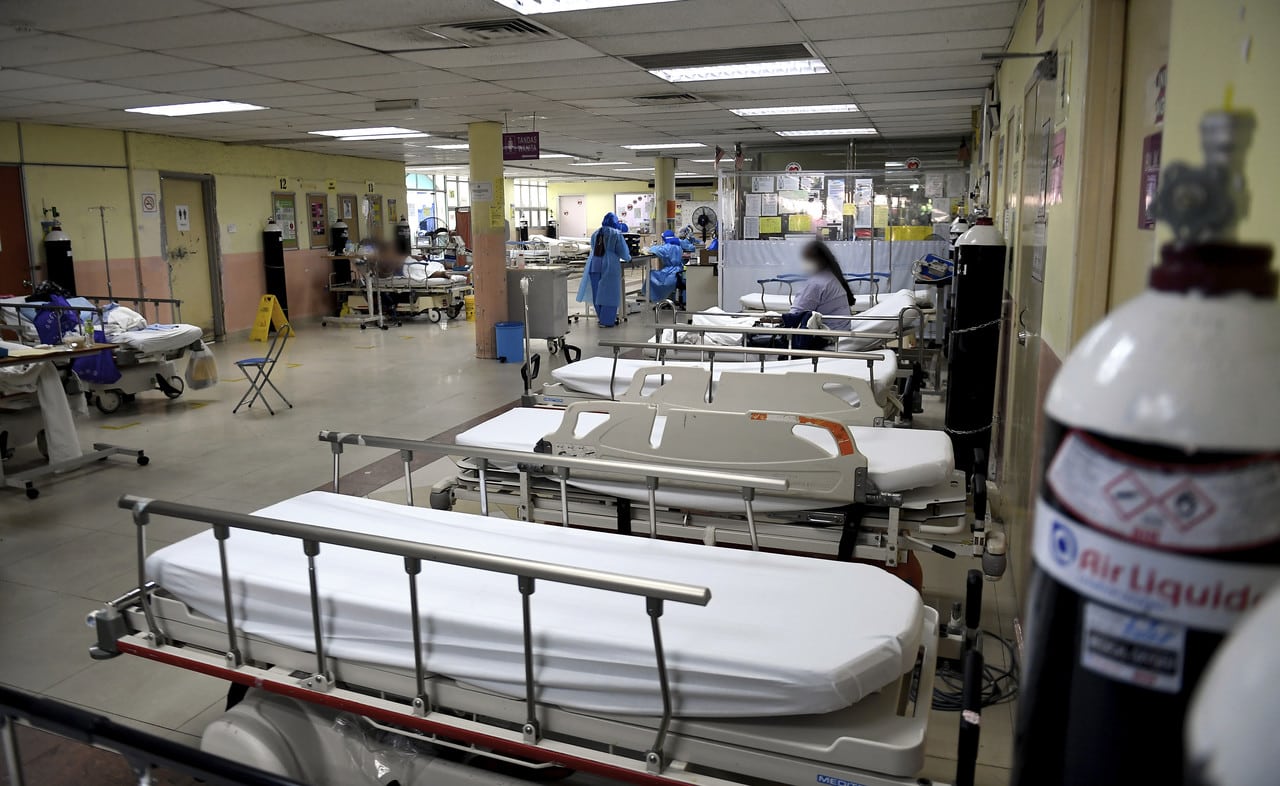
SHAH ALAM, Mar 13 — Greater collaboration between the public and private healthcare sectors is needed to address chronic underfunding and a shortage of specialist doctors in Malaysia’s public health system, said medical experts.
Public health medical specialist Prof Dr Sharifa Ezat Wan Puteh said that while the national healthcare system has achieved significant outcomes, structural challenges like budget constraints and manpower shortages continue to place strains.
“I do agree that the Health Ministry (MOH) is, in many ways, chronically underfunded, with its budget accounting for just around four to five per cent (of total government spending), which is relatively low.
“The second barrier is we have enough hospitals, but they are not running at the level we want,” she said during the Taxation, Public Finances, and Healthcare Funding forum at Hospital Universiti Kebangsaan Malaysia (HUKM) in Cheras today.
Despite the constraints, Dr Sharifa, who is from UKM’s Public Health Department, said the country’s healthcare indicators have steadily improved over the decades.
“Our life expectancy has increased. During the colonial era, we might only live up to 50 or 54, but today many reach 70, 80, or even older,” she said, adding that this change reflects Malaysia’s transition towards an ageing society.
Dr Sharifa highlighted Malaysia’s universal health coverage system, which ensures access to basic healthcare for all, including lower-income groups such as farmers, enabling them to receive essential treatments and medicines.
However, the system is facing mounting pressure due to shortages of specialist doctors and limited hospital capacity.
“Many specialist doctors, after completing training, leave the government sector. While some remain, I would say about a third leave for the private sector,” she said.
The migration of specialists to private practice has forced the government to explore new ways to retain talent, including allowing private services within public hospitals and introducing incentives.
Despite this, Dr Sharifa acknowledged that the private sector plays a crucial role in easing the burden on public health facilities.
“Without the private sector, the public sector is going to be highly burdened, and we need the private sector to work with us,” she said.
Dr Sharifa noted that the government is exploring ways to improve access to private healthcare through initiatives such as micro-insurance schemes under the Medical and Health Insurance/Takaful (MHIT) framework, especially for middle-income groups.

Public-private partnership crucial
Another speaker, endocrinologist Dr Azraai Bahari Nasruddin, said financial constraints and bureaucratic processes contribute to delays in expanding public healthcare infrastructure.
Requests for development funding from hospitals and clinics undergo several layers of filtering before reaching the national budget stage, often leaving many proposals unfulfilled.
“It is very clear why a lot of hospitals and clinics are disappointed at the end of the year,” he said, observing that the current revenue collected from patient charges is minimal compared to the overall cost of running the healthcare system.
“In 2024, we had 2.5 million hospital admissions and 46 million outpatient visits, but the total revenue collected was about half a billion ringgit; just over one per cent of the actual spending budget,” Dr Azraai added.
While some argue for fully free healthcare, he said a small charge can encourage patients to value medical services and reduce wastage.
“Some years ago, I wondered why we even bothered collecting fees. We have people queuing to pay RM1 to RM5 (for registration), so why not skip the queues and make it free at the source?
“For many years, that was what I felt, but my view has changed. I still think the concept of free healthcare at the point of service is a great idea, but I do not think it’s entirely right.
“Part of the reason is that everyone should share responsibility for their health,” Dr Azraai said.
Since public healthcare is highly subsidised, many people tend to take it for granted, with missed appointments reaching as high as 30 to 40 per cent in some cases.
He also pointed to workforce challenges, noting that while Malaysia has significantly improved the doctor-to-population ratio — from one to 1,300 to about one to 400 — the country still lacks sufficient senior specialists.
As private healthcare continues to expand, policymakers must focus on better integration between the two sectors.
“I believe public-private partnership should be reciprocal, benefiting both sides,” Dr Azraai said, suggesting that private healthcare professionals also contribute to training and providing services in the public sector.